What you Need to Know About the Latest Mental Health Data
What you Need to Know About the Latest Mental Health Data
The National Health Interview Survey (NHIS) was established in 1957 to monitor health issues throughout the U.S. Personal interviews are conducted with households across the nation on a wide range of health topics. The results of the annual surveys serve to inform achievement of national health objectives by tracking health status and health care access. In 2019 the questionnaire was redesigned to meet evolving need of those who use the data. The results of the redesign included improved measurement of health topics, shortened length of the questionnaire to make it less burdensome for participants, allow for better congruence with related data from other federal health surveys, provide structure for both ongoing and periodic topics, and integrate the latest advances in survey methodology and measurement (National Center for Health Statistics, 2021). A short video on the redesigned questionnaire is available for viewing using the following QR Code or by following the link:

Some of the Survey Reports and Data linked to NHIS include (with links for easy access:
- Early Releases of Selected Estimates from the NHIS
- Data Briefs
- National Health Statistics Reports
- Summary Health Statistics
- MMWR QuickStats
- Health E-Stats
- MMWR Reports
- NHIS-related information appears in select Vital and Health Statistics Reports, Series 1, Series 2 and Series 10.
- Advance Data
- Public Health Service Publications
- List of Articles Using NHIS Data
- Survey Procedures, Sample Design, Variance Estimation, and Other Methodological Studies
NCHS Releases New Mental Health Data for 2020
Key findings published by the NCHS in October 2021 show that nearly 20% of adults in the U.S. received mental health treatment during the past 12 months (Terlizzi & Norris, 2021), and included the following:
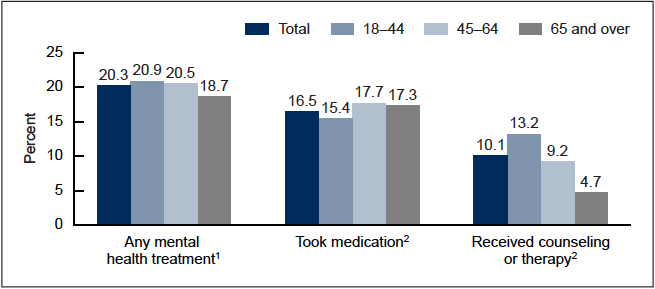
- 20.3% of adults received mental health treatment in the past 12 months. 16.5% took prescription medication for mental health issues and 10.1% received counseling or therapy from a mental health professional (Figure 1; Data Table for Figure 1 );
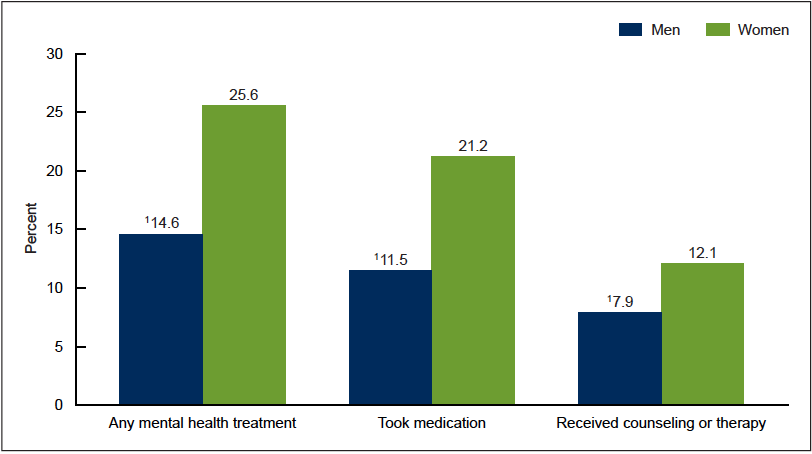
- More women than men received mental health treatment (Figure 2; Data Table for Figure 2);
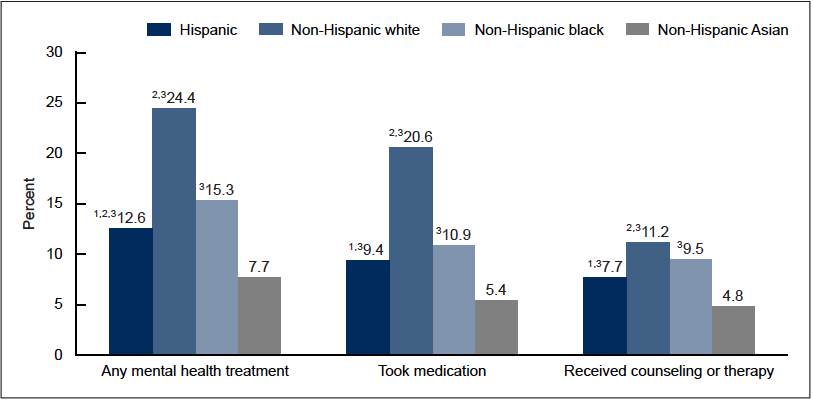
- Non-Hispanic white adults received any mental health treatment, compared to 15.3% of non-Hispanic black, 12.6% of Hispanic, and 7.7% of non-Hispanic Asian adults (Figure 3; Data Table for Figure 3);
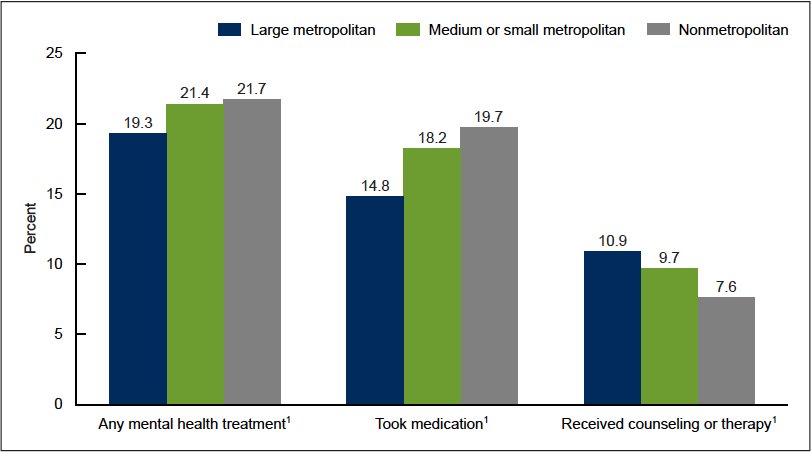
- The percentage of adults who took medication for mental health increased for those in less urban areas and conversely the percentage of those receiving counseling or therapy for mental health decreased (Terlizzi & Norris, 2021) (Figure 4; Data Table for Figure 4).
View the full NCHS Data Brief No. 419, October 2021.
Implications of These New Data
Few will be surprised that the percentage of those seeking mental health treatment has risen. More likely it is confirmation of what most people suspected, given the trauma of our country and the world since early 2020. What can the increase mean for behavioral health providers? Some of the consequences of the increased incidence of mental health issues can be:
- Unmet mental health needs – According to the MMRW (April 2, 2021), increases in mental illness such as depression and anxiety may mean unmet needs. Outbreaks of diseases such as the COVID-19 pandemic often mean increased fear and grief, social restrictions, limited ability of businesses to operate normally, unemployment or underemployment. The increase in depressive or anxiety disorders and treatment seeking behaviors are the natural result of these factors. Those with unmet treatment needs increased significantly during the height of the pandemic.
- Increased racial and ethnic disparities – Data from the MMRW (February 5, 2021) shows that racial and ethnic minorities are experiencing increases in mental health, substance misuse, inadequate food and unstable housing. Three times more Black persons and twice as many Hispanic persons than White persons reported not having enough food. Inadequate access to housing, food, and transportation constitutes a barrier to accessing treatment needed to address psychosocial stress and resultant mental health conditions or substance misuse
- Increased substance use and suicidal ideation – The impact of the pandemic during the first half of 2020 resulted in 40% of U.S. adults struggling with mental health or substance use, as reported in the MMRW (August 14, 2020). Anxiety/Depression symptoms were experienced by 31% of those polled; 13% began or increased substance use; 26% had trauma or stressor-related disorder symptoms; and 11% seriously considered suicide.
How To Meet the Needs of Those in Need
- One of the first steps might be to be aware of the data showing the consequences of the pandemic that are shared not only across the U.S., but around the world. A good way to begin is to read The “COVID-19 Effect” on Substance Use and Mental Health Disorders Catalyst blog post from December 9, 2020 that outlines how COVID-19 has changed the behavioral health landscape. In addiction to facts and figures about how the pandemic is manifesting in our communities, there is a list of consequences that may include some that had not been thought of before. Implications for those in recovery and information for how behavioral health providers might respond are two more topics that are covered.
- Ways behavioral health providers can help their clients are suggested and resources providers can access can be found in the Catalyst blog post Coping with a Pandemic: How Behavioral Health Providers Can Help Clients with Mental and Substance Use Disorders Meet the Challenges of COVID-19.
- What We Know So Far About the Impact of COVID-19 on Behavioral Health and Services describes how the pandemic has impacted behavioral health and services in general, by creating barriers to services. Resources and links are provided to help providers overcome these barriers. Another relevant article that addresses the barriers encountered by rural clients is Breaking Down Barriers to Treatment: Reaching Parity for Rural Clients with Co-occurring Substance Use Disorders and Serious Mental Illness. The post describes the wide range of barriers to treatment faced by those in rural areas and provides many links and resources for overcoming them.
- Addressing the many types of trauma encountered during the pandemic is the topic of The Impending Necessity of Trauma-Informed Care in Behavioral Health Services Due to COVID-19 (Coronavirus), a post that defines trauma and its effects and outlines what behavioral health providers can do to meet the needs of clients during this trying time.
While many will read of the latest data and feel alarmed or simply discouraged, the one sliver lining to the cloud of the pandemic has been the positive and creative response of many to the stress and barriers it has created. Federal agencies and researchers have increased flexibility to allow telehealth to expand, medication-assisted treatment to evolve according to needs, and data is being analyzed at an increased rate to inform providers and the public as quickly as possible. Caring people from every field have shared strategies for stress-reduction and coping as never before. While the negative impacts of the pandemic are often quite obvious, a Pew Research Center study has revealed a few positive impacts as well. While 41% missed family and friends, 33% mentioned they were able to spend more time with their families or have connected regularly using technology. As 32% of those surveyed described how the pandemic limited their activities, 26% developed new hobbies, new ways of doing things, or simply relaxed. Although 23% said the pandemic negatively impacted their job or career, 13% considered being able to work from home more productive and achieved greater balance between work and home life. For a more balanced perspective of the impact of COVID-19, read about the study on the Pew Research Center webpage.
Your Turn: Does the new data surprise you? How has the pandemic impacted you and your work? Please share your thoughts in the comments below.
Relevant articles from the Catalyst Blog: “Self-care” articles
US Department of Health and Human Services/Centers for Disease Control and Prevention MMWR:
Morbidity and Mortality Weekly Report (MMWR)
National Center for Health Statistics (NCHS)
NCHStats – A Blog of the National Center for Health Statistics
References
Czeisler MÉ, Lane RI, Petrosky E, et al. Mental health, substance use, and suicidal ideation during the COVID-19 pandemic—United States, June 24–30, 2020. MMWR Morb Mortal Wkly Rep 2020;69:1049–57. https://doi.org/10.15585/mmwr.mm6932a1external icon PMID:32790653
McKnight-Eily LR, Okoro CA, Strine TW, et al. Racial and ethnic disparities in the prevalence of stress and worry, mental health conditions, and increased substance use among adults during the COVID-19 pandemic—United States, April and May 2020. MMWR Morb Mortal Wkly Rep 2021;70:162–6. https://doi.org/10.15585/mmwr.mm7005a3
Terlizzi EP, Norris T. Mental health treatment among adults: United States, 2020. NCHS Data Brief, no 419. Hyattsville, MD: National Center for Health Statistics. 2021. DOI: https://dx.doi.org/10.15620/ cdc:110593.
Vahratian A, Blumberg SJ, Terlizzi EP, Schiller JS. Symptoms of Anxiety or Depressive Disorder and Use of Mental Health Care Among Adults During the COVID-19 Pandemic — United States, August 2020–February 2021. MMWR Morb Mortal Wkly Rep 2021;70:490–494. DOI: http://dx.doi.org/10.15585/mmwr.mm7013e2
This article was developed by Stephanie Asteriadis Pyle, PhD at CASAT, feel free to use, link to, or distribute this information. A link to our site and attribution would be much appreciated. Suggested citation:
Asteriadis Pyle, S. (2021, November 4). What you need to know about the latest mental health data. CASAT OnDemand. Retrieved November 12, 2021, from https://casatondemand.org/2021/11/03/what-you-need-to-know-about-the-latest-mental-health-data/.
Blog Post Tags:
Related Blog Posts
Related Learning Labs
Related Resources
.
- Buscar Tratamiento de Calidad para Trastornos de uso de Sustancia (Finding Quality Treatment for Substance Use Disorders Spanish Version)
- Finding Quality Treatment for Substance Use Disorders
- Focus On Prevention: Strategies and Programs to Prevent Substance Use
- Monthly Variation in Substance Use Initiation Among Full-Time College Students
- The National Survey on Drug Use and Health (NSDUH) Report: Monthly Variation in Substance Use Initiation Among Adolescents








