Two New Publications About Youth that Everyone Needs to Know About!
Two New Publications About Youth that Everyone Needs to Know About!
On October 26, 2021 SAMHSA published a new resource guide Preventing Marijuana Use Among Youth. The publication is a review of the literature on marijuana use prevention for youth, translates current research into tools and strategies for practitioners, and gives examples of ways prevention practitioners might implement them. An analysis and highlights of the document can be found below.
Preventing Marijuana Use Among Youth – Analysis and Highlights
Some important facts to note about terms in the guide are:
- For this document, “Youth” and “adolescents” are people aged 12-17, when the brain is still developing.
- The strategies in the guide are intended for use in states, communities, those in the prevention workforce, and other stakeholders. Examples of key stakeholders include policy makers, coalitions, businesses, educators and school administrators.
- The guide was written with the understanding that policies and legalization efforts surrounding marijuana are ongoing and availability is likely to increase.
- The strategies presented in the document are focused on youth as the evidence suggests that early use of marijuana is linked to the most significant damage.
The premise of the document is that marijuana use among youth is a public health concern because research shows that heavy and/or regular marijuana use may impair learning, may result in physical changes in parts of the brain governing attention and memory, and may result in higher risk of psychiatric conditions and substance use disorders (SUDs) (SAMHSA, 2021). Moreover, marijuana use by adolescents has been associated with poor school performance, increased dropout rates, suicidal ideation and behavior, and reduced male fertility.
The widespread availability of marijuana comes from both illegal and state-regulated sales and is affected by increased use and legalization of both medical and non-medical use, mass commercialization, higher potency, and greater variety of ingestion methods that result in highly variable and unpredictable levels and composition of cannabinoids in products that may be inhaled, applied topically, or otherwise ingested (SAMHSA, 2021). The guide presents in depth examination of the many available forms of marijuana, mechanisms of use, prevalence, and the short-term and long-terms harms caused by its use.
The prevention foundation used in the guide is the Socio-Ecological Model, shown below, that identifies the factors that protect youth from marijuana use or put them at risk for use at the individual, family, and community levels (SAMHSA, 2021).
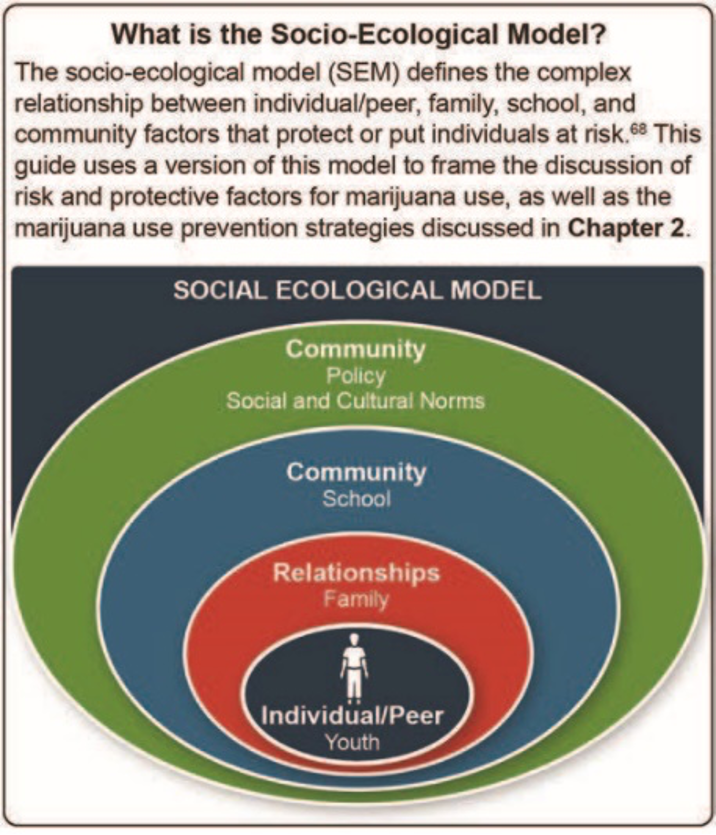
Figure 1: The socio-Ecological Model (SAMHSA, 2021).
Current challenges to Prevention efforts cited in the guide include:
Different regulatory structures across the country where marijuana ranges from illegal, legal for medical use only, or legal for recreational use, with legalized, non-medical use of marijuana for adults over 21 in 17 states and territories;
- Increasing public acceptance;
- Reduced perception of risk of marijuana use;
- Diverse types of marijuana products;
- Widespread marketing of marijuana.
State policies regulating marijuana vary widely and states may limit amounts of purchase each day; may have restrictions on advertising potency, or product design; may have disparate quality standards and health warnings; may limit the type and number of businesses that may sell marijuana or may impose restriction on delivery by retailers.
The rest of the guide contains the real “meat” of the document, describing the current research base for marijuana prevention in youth, comprehensive approaches to prevention, and a detailed list of prevention interventions with descriptions, age of target populations, and expected outcomes. Community level interventions and environmental strategies are described in detail, including packaging, marketing, taxation, and price regulation. A short chapter is devoted to guidance for selecting and implementing evidence-based policies and practices, interfacing programs with the Strategic Prevention Framework, and a comprehensive list of implementation guides and manuals, and another short chapter contains examples of comprehensive programs implemented in selected states. Evaluation and quality improvement is the final chapter, underscoring the critical need for program evaluation and subsequent quality improvement. Types of evaluation and study designs are presented, along with outcomes and appropriate indicators for measuring both long and short-term program outcomes, links to available national, state, and regional data sources, and a variety of evaluation resources.
Preventing Marijuana Use Among Youth is a primer on Marijuana prevention with a wealth of information and resources that outlines the steps and important considerations for undertaking the task of limiting marijuana use among youth throughout the U.S.
On December 7, 2021, the U.S. Surgeon General Dr. Vivek Murthy issued a statement urging a swift response to the mental health crisis among our nation’s youth that has been made much worse by the stressors of the COVID-19 pandemic. Highlights of the newly released Protecting Youth Mental Health: The U.S. Surgeon General’s Advisory will be found below.
The Surgeon General stated that “Mental health challenges in children, adolescents, and young adults are real and widespread. Even before the pandemic, an alarming number of young people struggled with feelings of helplessness, depression, and thoughts of suicide — and rates have increased over the past decade.” Surgeon General Murthy spoke of the alterations to the experiences of children, adolescents, and young adults in their home, school, and community environments and the importance of working together during the dual pandemic and mental health crisis.
Leading up to the COVID-19 pandemic, “ up to 1 in 5 children ages 3 to 17 in the U.S. having a mental, emotional, developmental, or behavioral disorder. Additionally, from 2009 to 2019, the share of high school students who reported persistent feelings of sadness or hopelessness increased by 40%, to more than 1 in 3 students. Suicidal behaviors among high school students also increased during the decade preceding COVID, with 19% seriously considering attempting suicide, a 36% increase from 2009 to 2019, and about 16% having made a suicide plan in the prior year, a 44% increase from 2009 to 2019. Between 2007 and 2018, suicide rates among youth ages 10-24 in the U.S. increased by 57%, – PDF and early estimates show more than 6,600 suicide deaths – PDF among this age group in 2020.” (HHS Press Office press release, December 7, 2021)
Many factors can shape the mental health of young people at the individual, family, community, environment, and societal levels. From social and economic inequalities, access to healthy food, relationships with peers, teachers, mentors, and parents, to the individual characteristics children are born with, mental health and well-being is everyone’s concern. The issues cannot be addressed unless all sectors of influence are part of the solution. The recommendations for supporting the mental health of children, adolescents, and young adults contained in the advisory include the following segments of society all stepping up to the plate:
- Young people themselves
- Family members and caregivers
- Educators, school staff, and school districts
- Health care organizations and health professionals
- Media organizations, entertainment companies, and journalists
- Social media, video gaming, and other technology companies
- Community organizations
- Funders and foundations
- Employers
- Federal, state, local, and tribal governments
Within the Surgeon General’s Advisory there are recommendations for those in each segment or sector to learn about the risk factors contributing to youth mental health symptoms, to learn to recognize groups that are at increased risk of mental health challenges, and to act. According to the Advisory, and to paraphrase, we must all:
- “Recognize that mental health is an essential part of overall health;
- Empower youth and their families to recognize, manage, and learn from difficult emotions;
- Ensure that every child has access to high-quality, affordable, and culturally competent mental
- health care;
- Support the mental health of children and youth in educational, community, and childcare
- Settings;
- Address the economic and social barriers that contribute to poor mental health for young
- people, families, and caregivers;
- And increase timely data collection and research to identify and respond to youth mental health
- needs more rapidly” (Protecting youth mental health – hhs.gov 2021).
The Advisory contains detailed strategies for each sector and lists of resources to assist them by acting. Although there is a solid research base, there is also the acknowledgement that additional research is needed and some of the most pressing topics for future research are identified.
The Surgeon General concludes the Advisory by stating that the changes that need to be made will require time and effort as well as structural changes and addressing stigma log associated with mental health issues. But the result will be a “more comprehensive, more fulfilling, and more inclusive vision of what constitutes public health” (Protecting youth mental health – hhs.gov 2021).
Additional Resources may be found in the CASAT OnDemand Resources & Downloads section.
Your Turn: Do your experiences in the prevention of youth marijuana use or mental health mirror the latest research or are they different? Share your perspective in the comments below.
References
Office of the Surgeon General. (n.d.). Protecting youth mental health – hhs.gov. Protecting Youth Mental Health: The U.S. Surgeon General’s Advisory . Retrieved December 9, 2021, from https://www.hhs.gov/sites/default/files/surgeon-general-youth-mental-health-advisory.pdf. Substance Abuse and Mental Health Services Administration (SAMHSA).
Preventing Marijuana Use Among Youth. SAMHSA Publication No. PEP21-06-01-001. Rockville, MD: National Mental Health and Substance Use Policy Laboratory. Substance Abuse and Mental Health Services Administration, 2021.
This article was developed by Stephanie Asteriadis Pyle, PhD at CASAT. Feel free to use, link to, or distribute this information. A link to our site and attribution would be much appreciated. Suggested citation:
Asteriadis Pyle, S. (2021, December 9). Two new publications about youth that everyone needs to know about! CASAT OnDemand. Retrieved December 9, 2021, from https://casatondemand.org/2021/12/09/two-new-publications-about-youth-that-everyone-needs-to-know-about/.
Blog Post Tags:
Related Blog Posts
Related Learning Labs
Related Resources
.
- Buscar Tratamiento de Calidad para Trastornos de uso de Sustancia (Finding Quality Treatment for Substance Use Disorders Spanish Version)
- Finding Quality Treatment for Substance Use Disorders
- Focus On Prevention: Strategies and Programs to Prevent Substance Use
- Monthly Variation in Substance Use Initiation Among Full-Time College Students
- The National Survey on Drug Use and Health (NSDUH) Report: Monthly Variation in Substance Use Initiation Among Adolescents








