Exploring the Interplay of Social Determinants: A Deeper Dive into Hunger, Homelessness, and Behavioral Health
Editor’s Note: This post was originally published in November 2021 and has been updated to reflect current trainings.
The Overall Scale of Hunger and Homelessness in the United States
Certain populations in the United States (U.S.) are at a heightened risk of homelessness compared to the general population, and this risk is significantly associated with gender, race, and ethnicity. Men and people of color are disproportionately affected, exhibiting a higher vulnerability than women and white individuals.
According to the Hunger & Homelessness Awareness Week website, the facts are that in the U.S.:
- 37.2 million Americans live below the poverty line
- 2 Million American live below the poverty level
- 580,000 Americans are normless on any given night
- 44 million Americans risk suffering from hunger
- 1 in 6 American children live in poverty
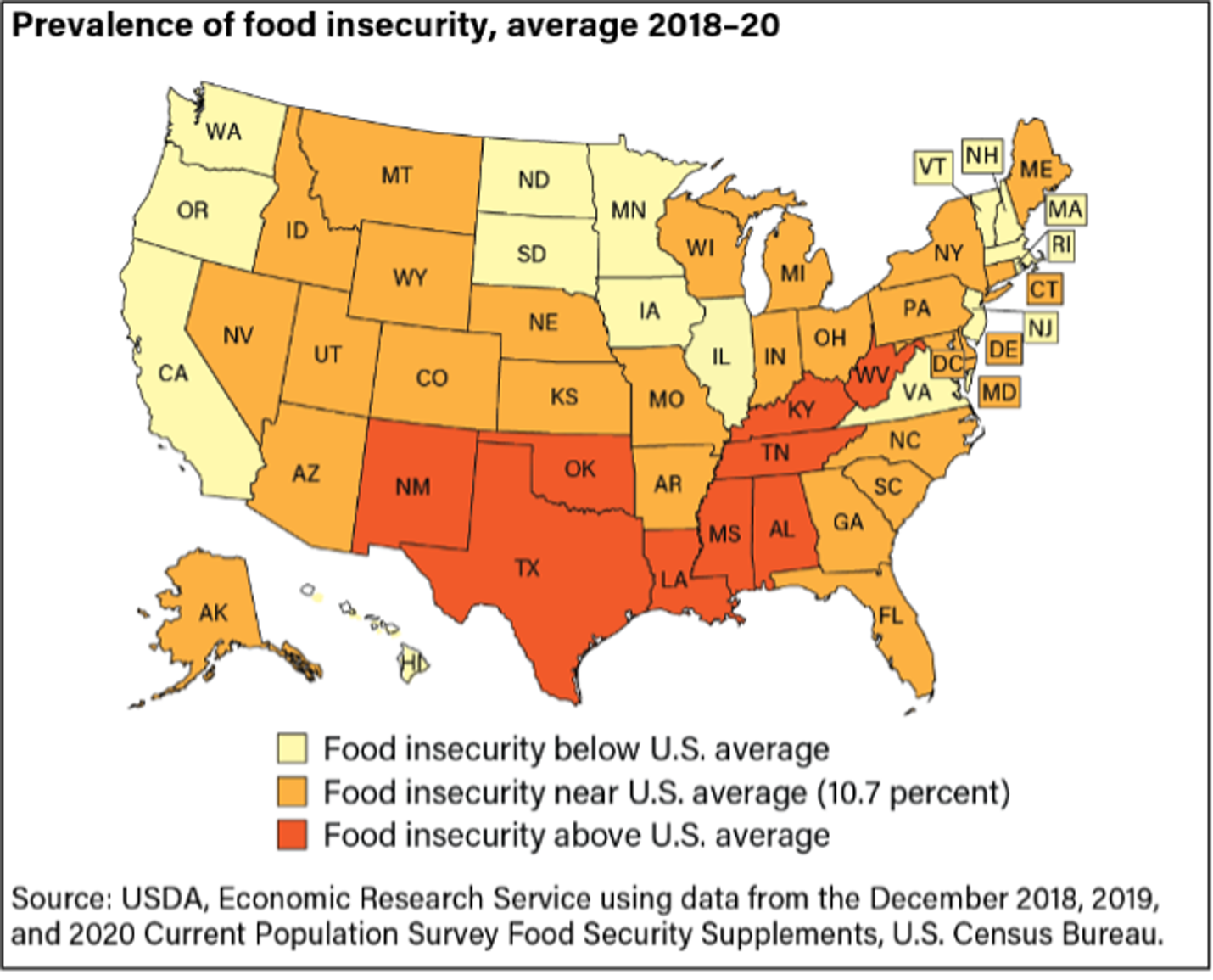
Image text description: Map of the United States showing food insecurity above average in: NM, TX, OK, LA, MS, AL, TN, KY, WV; Food insecurity near U.S. average (10.7%) in: NV, ID, MT, WY, UT, CO, AZ, NE, KS, MO, AR, WI, MI, IN, OH, PA NY, ME, CT, DE, DC, MD, NC,, SC, GA, FL; Remaining states are below U.S. average: WA, OR, CA, ND, SD, MN, IA, IL, VA, VT, NH, MA, RI, NJ, VA
Source: USDA, Economic Research Service using data from December 2018, 2019, and 2020 Current Population Survey Food Security Supplements, U.S. Census Bureau.
In Nevada, homelessness is a pressing issue, ranking 9th in the United States with an estimated rate of 23.3 homeless individuals per 10,000, exceeding the national average of 17 per 10,000 (Porch Research, 2021). U.S. Housing and Urban Development (HUD) data reveals that among the homeless population in Nevada, 53.1% were living unsheltered, and 10% were considered chronically homeless. Meanwhile, the state grapples with a food insecurity rate of 12.7%, closely aligning with the national average of 10.7% (R.W. Johnson State of Childhood Obesity, 2021). The characteristics associated with higher rates of food insecurity in Nevada include households led by a single woman, individuals living alone, Black non-Hispanic and Hispanic households, those with an income-to-poverty level of 1.85 and lower, and households in principal cities of metropolitan areas and nonmetropolitan areas (USDA, 2022). These statistics highlight the complex challenges faced by the state’s residents, encompassing both housing instability and food insecurity.
Impact of Hunger and Homelessness
The significant impact of food and housing insecurity in the U.S. is heightened by the widespread experience across various age groups, races, and ethnicities. This becomes especially noteworthy when considering them as two of the Social Determinants of Health, alongside Economic Stability, Education, Community and Social Context, and the Health Care System.
Some of the more direct impacts of hunger and homelessness include:
- Impacts on health – Chronic diseases such as diabetes and high blood pressure are obvious consequences of a poor or inadequate diet, but others such as kidney disease, eye disease, heart disease, and obesity are not as obvious. People with food insecurity can also have more psychological and behavioral health issues and children may have school problems or struggle in social situations. Lack of access to appropriate food disproportionally affects the physical and mental health of young children, sometimes delaying development. Research shows that chronic illnesses like asthma and anemia and problems such as hyperactivity, anxiety, and aggression in young children are linked to food insecurity (Feeding America, 2021). The health impacts go even further, singling out those with Substance/Opioid Use Disorder (SUD/OUD) in the following ways:
- People with substandard living conditions or who live in counties with very low levels of social capital have been shown by research to have the highest overdose rates. Substance use and poverty are reinforced by untreated mental health disorder and a shortage of stable housing and are correlated with OUD in underserved communities (Opioid Response Network, 2021).
- People with SUD/OUD and insecure housing and food have unique barriers to prevention due to lack of protective factors such as lack of access to primary care and the stressful environment created by poverty.
- People with SUD/OUD have barriers to appropriate care, engagement, and retention in treatment that can include lack of access to evidence-based care from either lack of availability or lack of transportation, lack of providers qualified to administer medication for SUD or OUD, fear or mistrust of the medical system due to prejudice or stigma during previous encounters, or lack of insurance or coverage for treatment (Opioid Response Network, 2021).
- People in recovery from SUD and OUD may not receive proper screening and testing or support for recovery due to either being homeless or not having safe shelter or living conditions. People in recovery also frequently have co-occurring disorders and prioritize food and shelter needs above higher level needs (Opioid Response Network, 2021).
What the Research Says About the Impact of Hunger and Homelessness on SUD, OUD, and SMI
Substance Use Disorder (SUD), Opioid Use Disorder (OUD), and Serious Mental Illness (SMI) are highly impacted by Social Determinants of Health. The current base continues to grow, as we seek to understand effective responses for behavioral health providers on the front lines who are working to address the problem. A recent study investigated the trajectories of food insecurity among homeless adults who took part in a housing intervention trial. The researchers aimed to determine whether individuals receiving the intervention, particularly those with specific mental and substance disorders, exhibited predictable patterns of food insecurity over time. The study identified four distinct food insecurity trajectories: persistently high, increasing, decreasing, and consistently low food insecurity. Participants in the study had at least one alcohol or other substance use disorder and one non-substance-related mental disorder, such as a major depressive episode, mood disorder with psychotic features, substance disorder, or co-occurring disorder. The findings revealed a strong association between homeless individuals with major depressive episodes, mood disorders with psychotic features, substance disorders, or co-occurring substance use or alcohol use disorders along with a non-substance-related mental disorder, and membership in the persistently high food insecurity trajectory group (Lachaud et al., 2020). This research underscores the inadequacy of solely providing housing in addressing homelessness and hunger. It emphasizes the necessity for more comprehensive programs, services, and resources that integrate mental health services with meeting basic needs for food and housing security.
There is a complex interplay that impacts the health and well-being of individuals. The prevalence of food insecurity and homelessness sheds light on the complex dynamics of housing instability and insufficient access to nourishment. The far-reaching consequences of these challenges extend beyond physical health, affecting mental and behavioral well-being, with specific implications for those grappling with Substance Use Disorder (SUD), Opioid Use Disorder (OUD), and Serious Mental Illness (SMI). Research indicates the need for holistic approaches that integrate mental health services with fundamental necessities like food and housing security. As we confront these complex issues, it becomes imperative to address the root causes and implement comprehensive programs that offer sustainable solutions, bridging the gap between behavioral health and basic human needs.
Resources
- Food Bank of Northern Nevada – 1 in every 9 Nevadans facing hunger every day, people you see every day are fighting this fight.
- Food for Thought – dedicated to helping hungry children in our community by providing food, as well as solutions, resources and increased awareness, to combat hunger.
- Las Vegas Rescue Mission – We work around the clock to assist those who need the most help in our community.
- Catholic Charities of Southern Nevada – We give help and hope to more than 4,200 vulnerable men, women and children each day, regardless of religion, in southern Nevada by feeding, sheltering and transforming lives.
- CASAT OnDemand: Now you can find the information you need and access it instantly any time of the day or night – any time you have the time.
- Catalyst Blog – is the simple solution to your behavioral health information needs. We sort through the most recent material for you, and re-purpose, revise, or transform it into byte sized, easily digested information morsels so you can make sense of it all. If we can’t find it, we will create it.
- CASAT Conversations – is a podcast dedicated to exploring behavioral health topics. Season 3 is dedicated to health equity. Listen today!
- Feeding America – What hunger looks like in Nevada
- Opioid Response Network – Supporting substance use disorder treatment, prevention and recovery resources
- Brandeis Opioid Resource Connector – How Social Determinants of Health Create Differential Impacts
- Addiction Technology Transfer Center Network (ATTC) – Emerging Issues Around COVID-19 and Social Determinants of Health for the Substance Use Prevention, Treatment, and Recovery Workforces
- Substance Abuse and Mental Health Services Administration (SAMHSA):
- Homelessness Programs and Resources
- Grants Programs and Resources for Homelessness
- Behavioral Health Equity
- Key Statistics & Graphics on Food Security in the U.S.
- Food & Nutrition Assistance
- The National Alliance to End Homelessness – a nonpartisan organization committed to preventing and ending homelessness in the United States.
References
Mental and substance use disorders and food insecurity among homeless adults participating in the At Home/Chez Soi study Lachaud J, Mejia-Lancheros C, Wang R, Wiens K, Nisenbaum R, et al. (2020) Mental and substance use disorders and food insecurity among homeless adults participating in the At Home/Chez Soi study. PLOS ONE 15(4): e0232001. https://doi.org/10.1371/journal.pone.0232001
Opioid Response Network/SAMHSA. (2021). Brandeis Opioid Resource Connector. The Opioid Epidemic and COVID-19: How Social Determinants of Health Create Differential Impacts Brandeis Opioid Resource Connector. Retrieved November 18, 2021, from https://opioid-resource-connector.org/resources/opioid-epidemic-and-covid-19-how-social-determinants-of-health-create-differential.
Blog Post Tags:
Related Blog Posts
Related Learning Labs
Related Resources
.
- Buscar Tratamiento de Calidad para Trastornos de uso de Sustancia (Finding Quality Treatment for Substance Use Disorders Spanish Version)
- Finding Quality Treatment for Substance Use Disorders
- Focus On Prevention: Strategies and Programs to Prevent Substance Use
- Monthly Variation in Substance Use Initiation Among Full-Time College Students
- The National Survey on Drug Use and Health (NSDUH) Report: Monthly Variation in Substance Use Initiation Among Adolescents








