
National Prevention Week occurs during the third week in May because first time substance use by adolescents and full-time college students most frequently occurs in June or July (HHS, 2012; Lipari, 2015). (Tweet this!) Since May immediately precedes the beginning of summer, it is a good time for parents, schools, communities, and behavioral health professionals to focus on prevention.
SAMHSA’s National Prevention Week will be observed May 12-18, 2019 (Tweet this!) and is an observance each year designed to increase awareness of and action surrounding mental health disorders and substance use disorders. According to the National Prevention Week website, the three main goals are to:
- Involve communities in raising awareness about behavioral health issues and implementing prevention strategies, and showcasing effectiveness of evidence-based prevention programs;
- Foster partnerships and collaboration with federal agencies and national organizations dedicated to behavioral and public health; and
- Promote and disseminate quality behavioral health resources and publications.

For the entire week, each day has a theme to help focus on key topics in substance abuse and mental health disorders. The 2019 daily themes are:
- Monday, May 13: Preventing Prescription and Opioid Drug Misuse
- Tuesday, May 14: Preventing Underage Drinking and Alcohol Misuse
- Wednesday, May 15: Preventing Illicit Drug Use and Youth Marijuana Use
- Thursday, May 16: Preventing Youth Tobacco Use
- Friday, May 17: Preventing Suicide
Why Prevention?
The reasons for implementing substance use disorder and behavioral health disorder prevention interventions are many. Here are a just a few of them:
- The scope of the problem is huge and costly: By 2020, mental health and substance use disorders will surpass all physical diseases as a major cause of disability worldwide. (Tweet this!) The annual total estimated societal cost of substance use disorder in the US is $510.8 billion, with an estimated 23.5 million Americans aged 12 and older needing treatment for substance use. The cost of the country’s opioid crisis alone is estimated to have exceeded $1 trillion from 2001 to 2017, and is projected to cost an additional $500 billion by 2020, according to analysis released by Altarum, a nonprofit health research and consulting institute.
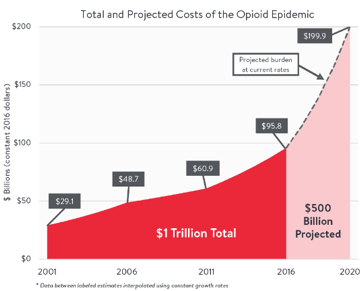
The costs are borne by individuals in the form of lost wages; the private sector in lost productivity and health care costs; and federal, state and local governments in lost tax revenue and additional spending on health care, social services, education and criminal justice, with an additional $500 billion projected costs by the year 2020. The emotional toll on individuals with a substance use disorder, and that on their families and communities is substantial and not quantifiable in any fiscal or monetary sense. How do you put a price on human pain and suffering?
- These disorders result in lost lives: Each year, approximately 5,000 youth under the age of 21 die as a result of underage drinking. More than 34,000 Americans die every year as a result of suicide, approximately one every 15 minutes. Half of all lifetime cases of mental health and substance use disorders begin by age 14 and three-fourths by age 24—in 2008, an estimated 9.8 million adults in the US had a serious mental illness.
- Further complicating the overall issue is the fact that many young people have more than one behavioral health disorder. An estimated 37% of people with alcohol use disorder and 53% of other drug disorders also have at least one serious mental illness. One in five individuals with a diagnosable mental health disorder also suffer from a substance use disorder. And it’s not always clear what leads to what.
- Mental health disorders, including substance abuse and dependence, are frequently associated with physical health disorders (O’Connell, 2009). Numerous studies support drinking alcohol as a risk factor for primary liver, breast, and colorectal (colon) cancer (National Cancer Institute, 2019). At least one selective review of the literature has also linked a higher prevalence of a lengthy list of physical health problems with severe mental illness (SMI), including, but not limited to, Tuberculosis, HIV, hepatitis, Obesity-related cancer, Osteoporosis, Poor dental status, Impaired lung function, Sexual dysfunction, Obstetric complications, Stroke, myocardial infarction, hypertension, and Obesity (De Hert, et. al, 2011).
- Substance use disorders also disproportionately affect certain groups of young people already identified as at-risk. Young people in the age range of 10-24 years are affected during the time in life when key transitions are occurring (Deganhardt, et. al, 2016; Squeglia & Gray, 2016). Some of the groups affected and just one example for each for the many ways they may be impacted are:
- Young people with mental health problems
- Substance use may worsen or cause a recurrence of symptoms
- Young people who identify as lesbian, gay, bisexual, transgender, and questioning (LGBTQ), or same-sex attracted
- More concerning than the fact that LGBTQ young people have higher overall rates of substance use than the general population is the fact that this group also exhibits less common and riskier patterns such as use of injectionable drugs and heroin
- Young offenders
- Prevalence of substance use disorders is higher in youth involved in criminal justice systems
- Indigenous young people
- Economic and social disadvantages, unemployment, homelessness, incarceration, and disruption of families may result in increased susceptibility to substance use and misuse
- Young People who are homeless
- Reduced access to social services, health care, and other support can exacerbate behavioral health and substance use disorders
- Young people who inject drugs
- This group bears the additional risk of early exposure to HIV and hepatitis C
About Substance Use Disorder Prevention
Prevention practitioners must be aware of these linkages and identify opportunities to address health in a more comprehensive way working across disciplines to prevent mental health and substance use disorders and promote wellness. Wellness means overall well-being and incorporates the mental, emotional, physical, occupational, intellectual, and spiritual aspects of a person’s life. Each aspect of wellness can affect overall quality of life, so it is important to consider all aspects of health. How do we define prevention so that we can approach it as a separate and distinct field from the treatment, recovery, and maintenance of recovery? Prevention is defined as actions that minimize or eliminate conditions known to contribute to a specific condition, problem, illness, or disorder. Establishing conditions that enhance opportunities to achieve healthy outcomes is critical. And most importantly, prevention occurs prior to the problem appearing or becoming serious or severe. In addition, substance use disorder prevention includes the following principles:
- Alcohol use is acceptable only for those of legal age and only when the risk of adverse consequences is minimal.
- Prescriptions and over-the-counter drugs are used only for the purposes for which they were intended.
- Other substances such as gasoline or aerosols are used only for their intended purposes.
- And finally, illegal drugs and tobacco are not used at all.
Prevention focuses on interventions that occur prior to the onset of a disorder and that are intended to prevent the occurrence of the disorder or reduce the risk for the disorder. Prevention involves activities that promote positive actions and behavior. We all take preventive actions every day: we wash our hands and brush our teeth to prevent disease; we wear seat belts and drive carefully to prevent injury in cars; and we eat good foods and get adequate rest to best maintain wellness. Taking preventative action is not an absolute guarantee, just as brushing our teeth doesn’t eliminate the possibility of getting cavities. Doing what we can to prevent problems lessens the likelihood of the problems occurring in the future. Substance abuse prevention works the same as any other prevention. Just as we know from research what puts people at risk for cavities or serious injury or death in a car crash, we know from research what puts people at risk for substance use disorders and we know what protects people from developing a substance use disorder. Reducing risks and enhancing protective factors is one of the keys to substance abuse prevention.
According to the Substance Abuse and Mental Health Services Administration (SAMHSA) and the Center for Substance Abuse Prevention (CSAP), prevention is “a proactive process which empowers individuals and systems to meet challenges of life events and transitions by creating and reinforcing conditions that promote healthy behaviors and life styles.” Prevention is collaborative, comprehensive action that leads to planned change which creates conditions that give persons the best chance of success in their lives and community. Examples of collaborative systems are coalitions and State epidemiological outcomes workgroups (SEOWS).
SEOWS include people such as epidemiologists, state and local officials, program planners, community stakeholders, and prevention practitioners who work together to collect, analyze, and disseminate substance use and behavioral health data. Workgroup members prepare a state epidemiological profile and then make data-driven decisions as they integrate the Strategic Prevention Framework (SPF) into their prevention planning. The Nevada Epidemiological Profile for 2018 is the most current one for the state. Other Substance Abuse Treatment and Prevention Agency (SAPTA) epidemiological profiles and behavioral health reports can be found on the Nevada Division of Public and Behavioral Health (DBPH) Office of Public Health Informatics and Epidemiology (OPHIE) website.
Community coalitions are organizations of individuals representing diverse organizations, factions or constituencies who agree to work together in order to achieve a common goal. Community prevention coalitions include members of communities at the local level, both individuals and representatives of organizations, and should reflect the diversity of the community and include Youth, Parents, Businesses, Media, Schools, Youth serving organizations, Local law enforcement, Religious organizations, Civic organizations, Healthcare professionals, and others. Nevada’s Statewide Coalition Partnership, its member coalitions, and the Northern Nevada Behavioral Health Coalition are coalition organizations that advocate actions, policies, and procedures to help shape the culture in Nevada in support of healthier lives.
For training on use of epidemiology for prevention purposes, the Prevention Technology Transfer Center Network (PTTC) has a link to a webinar from April 16, 2019 that was developed by the Mountain Plains PTTC. The webinar is entitled Informing Prevention: The Effective Use of Epidemiological Data and contains details for determining the scope of a problem for a specific target population. Viewers of this YouTube video will learn where to access and ways to analyze epidemiological data for prevention purposes.
No definition of prevention is complete without adding that its purpose is lost if it is not effective. There are no silver bullets in prevention. No single program will “do the trick” and there are no shortcuts. What exactly does the “effective” prevention definition mean? It means preventing substance use and mental health disorders is everyone’s problem, so everyone must be part of the solution. It means people representing all facets of each community need to be involved. Research supports the importance and effectiveness of comprehensive, community-based prevention approaches, especially environmental strategies (Holder, 2004; Mason, Fleming, and Haggerty, 2016; SAMHSA’s CAPT, 2009 ). A comprehensive approach to behavioral health also means seeing prevention as a distinct part of an overall continuum of care. Prevention is important especially for young populations because it is a way of identifying a range of risk factors for substance use disorder, behavioral health disorders and other problem behaviors and reducing them to diminish negative consequences that can impact the overall health and well-being for a lifetime.
The “Prevention Decade”
In 2015 the Institute of Medicine and National Research Council of the National Academies Forum on Promoting Children’s Cognitive, Affective, and Behavioral Health published Unleashing the Power of Prevention, a paper intended to inform and stimulate discussion among its participants. The work was developed for the American Academy of Social Work and Social Welfare’s Grand Challenges for Social Work Initiative in collaboration with the collation for Behavioral Health. In the paper, the authors proposed that for many years our response to behavioral health problems has been to wait until the problem has been identified and then treat it. (Hawkins, et.al., 2015). With 30 years of research, the authors contended, prevention science has reached critical mass and they challenged the field to commit to using this knowledge to create policies, program funding, and a workforce that would reduce both the incidence and prevalence of behavioral health problems among children and adolescents by 20 percent within ten years. Calling it “The Prevention Decade,” the forum proposed a two-pronged approach for population-wide reductions in behavioral health problems:
“1. Implement and sustain, at scale, effective universal promotion and preventive interventions designed to benefit all young people.
2. Provide and sustain, at scale, effective selective and indicated interventions that target children, adolescents, and young adults at elevated levels of risk or early stages of problem involvement (Hawkins, et. al. 2015).”
In addition, authors outlined seven outcomes with actionable outcomes with accompanying goals to achieve success for the “interdisciplinary and cross-sector collaboration” challenge, stating “It’s time to unleash the power of prevention by creating programs, training, and infrastructures that put prevention to work nationwide for all young people, resulting in healthier lives, families, communities, and economies. Prevention is the best investment we can make, and the time to make it is now (Hawkins, et. al. 2015).”
NPW 2019 Promo Video: This is Prevention. This is Changing Lives.
National Prevention Week (NPW) Promotional Materials
There are a variety of materials in the NPW Toolkit to help plan your NPW events and inspire others to participate. Some of the resources include:
- NPW promotional toolkit wristband
- NPW promotional videos
- NPW logos and stickers
- NPW web and print graphics
- Prevention resources from SAMHSA and other federal partners
- Webinars on NPW themes
- Reports on prevention topics
National Prevention Week (NPW) Events and Activities
Anyone can plan an event to participate in National Prevention Week. Some past events include:
- Organizing a health fair.
- Painting a school mural with a healthy living theme.
- Throwing an ice cream social as a stress-reducer on a college campus.
- Sponsoring a fun-run/walk with a prevention theme.
- Holding a moment of silence honoring prevention.
Joint the Prevention Challenge today. Learn more about how to participate in events in your community on social media. Sponsoring NPW events can show your community what you are doing for prevention, bring the community together, and inspire others to participate as well. (Tweet this!) The NPW Toolkit is available in English and Spanish to help you get started and SAMHSA can help promote your community’s event. More information can be found on the NPW Community Events page. Resources and materials for NPW 2019 can also be found in the Resources and Uploads section of CASAT OnDemand and include new and archived NPW webinars.
Effective prevention is a research-based, comprehensive, and collaborative effort, consisting of multiple strategies across multiple domains throughout the lifespan. (Tweet this!)
References
Degenhardt, L., Prof, Stockings, E., PhD, Patton, G., Prof, Hall, W. D., Prof, & Lynskey, M., Prof. (2016). The increasing global health priority of substance use in young people. Lancet Psychiatry, the, 3(3), 251-264. doi:10.1016/S2215-0366(15)00508-8
De Hert, M., Correll, C. U., Bobes, J., Cetkovich-Bakmas, M., Cohen, D., Asai, I., … Leucht, S. (2011). Physical illness in patients with severe mental disorders. I. Prevalence, impact of medications and disparities in health care. World psychiatry: official journal of the World Psychiatric Association (WPA), 10(1), 52–77.
Hawkins, J. D., J. M. Jenson, R. Catalano, M. W. Fraser, G. J. Botvin, V. Shapiro, C. H. Brown, W. Beardslee, D. Brent, L. K. Leslie, M. J. Rotheram-Borus, P. Shea, A. Shih, E. Anthony, K. P. Haggerty, K. Bender, D. Gorman-Smith, E. Casey, and S. Stone. 2015. Unleashing the Power of Prevention. NAM Perspectives. Discussion Paper, National Academy of Medicine, Washington, DC. doi: 10.31478/201506c
Holder, H. D. (2004). Community prevention of young adult drinking and associated problems. Alcohol Research & Health, 28(4), 245.
Lipari, R. N. (2015).https://www.samhsa.gov/data/sites/default/files/report_2049/ShortReport-2049.pdf (CBHSQ Report August 27, 2015). Washington, DC: Substance Abuse & Mental Health Services Administration, Center for Behavioral Health
Mason WA, Fleming CB, Haggerty KP. 2016. Prevention of marijuana misuse: School-, family-, and community-based approaches. In: Compton MT, editor. Marijuana and mental health. Arlington, VA: American Psychiatric Publishing
National Cancer Institute at the National Institutes of Health. Alcohol and Cancer Risk. (n.d.). Retrieved April 18, 2019, from https://www.cancer.gov/about-cancer/causes-prevention/risk/alcohol/alcohol-fact-sheet
SAMHSA’s CAPT, 2009. Information Sheet 1: A Behavioral Health Lens for Prevention, www.samhsa.gov/capt/sites/default/files/resources/behavioral-health-factsheet.pdf. this document was developed under the Substance Abuse and Mental Health Services Administration’s (SAMHSA) Center for the Application of Prevention Technologies contract. Reference #HHSS277200800004C.
Squeglia, L.M. & Gray, K.M. Curr Psychiatry Rep (2016) 18: 46. https://doi.org/10.1007/s11920-016-0689-y
Substance Abuse and Mental Health Services Administration (HHS). (2012). Monthly variation in substance use initiation among adolescents. the NSDUH report : National survey on drug use and health: The NSDUH report;2012 ASI 4096-10.213;NSDUH_080. ().
